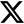Early in my life, I knew that I wanted to help people living with serious health issues. Part of this conviction came from my interest in science, research, and solving complex biological questions. The other motivating factor was the way my life changed after suffering a brain injury as a result of a severe concussion. For months, it was difficult to focus, retain memories, and process high-level concepts.
I am fortunate because I recovered and did not have lasting neurological effects, unlike many people who suffer neurological damage or have a condition like epilepsy. In those few short months, every part of my life was impacted. Now, when I hear stories from people living with epilepsy that they have trouble remembering, or miss activities because they are recovering from a seizure, or are struggling with depression and isolation, I reflect back on my own experience and have great empathy for these life-altering challenges.
My hope is that one day, we may cure epilepsy and give thousands of people experiencing seizures new options for achieving their ideal lives.
Driven by Science
UCB has a strong heritage in epilepsy and strong history in finding and developing the right molecules to treat the symptoms of the disease. One of the challenges, however, is that there are so many subtypes, impacting patients differently. Whether a person is experiencing focal seizures, seizure clusters, or a rare syndrome, their experience and response to medication varies. Insights from our research and development efforts have highlighted the need for potential new treatments in a number of epilepsy subtypes, such as tumor-associated epilepsy, tuberous sclerosis complex, and autoimmune epilepsy.
As we come to understand each of these epilepsy types, we come closer to being able to target the critical underlying pathologies, creating the potential for disease modification or correction at the genomic level.
To do this, it’s important that we continue to invest in research and development. UCB has a strong commitment to R&D, investing about a quarter of our revenue back into our science globally. We’re also using artificial intelligence and computational drug design to better understand and diagnose different epilepsies and predict the best course of treatment. Our decentralized clinical trial model helps maximize patient participation across diverse populations, and we employ data-driven digital targeting to recruit patients across all ages, sexes, races, and locations. This means that our trials will better match the population of people who experience epilepsy. Coupled with our collaborations, and acquisitions with biotech and gene therapy companies, our ambition is to impact the underlying causes of the disease and ultimately, cure epilepsy.
As part of that ambition, in March, we completed the acquisition of Zogenix, a global biopharmaceutical company commercializing and developing therapies for rare forms of epilepsy, including Dravet syndrome, Lennox-Gastaut syndrome, and CDKL5 Deficiency Disorder (CDD). Soon after the acquisition, we received FDA approval for a treatment option for seizures associated with Lennox-Gastaut syndrome.
LGS is a severe childhood-onset developmental and epileptic encephalopathy (DEE) characterized by drug-refractory seizures with high morbidity1 as well as serious impairment of neurodevelopmental, cognitive, and motor functions.2 LGS affects an estimated 30,000 – 50,000 patients in the U.S.3
Inspired by Patients
As we advance our science, we also need to consider the patient experience. Knowing that we need to partner to make a greater impact within the neurology ecosystem, we have multiple projects with leading medical centers to improve epilepsy care across the patient journey. We have also engaged in research that highlights the importance of social determinants of health related to epilepsy risk in certain populations.
For instance, Hispanics are one of the largest subpopulations of people living with epilepsy – more than 700,000 people – yet there are persistent discrepancies in their access to care, treatment, and patient outcomes compared with other populations.1-5 To better understand the experiences of Hispanic people with epilepsy and to improve our collective effort to break down barriers to equitable health outcomes, we are working with patients and their families to learn more about their experiences and what resources may be beneficial. A significant barrier uncovered during our research was misinterpretations due to language and culture. To address this care gap, our team created bilingual and culturally competent Spanish educational resources on epilepsy and our medications.6 This multi-phased research project has provided a way to better understand cultural attitudes and behaviors of Hispanic people with epilepsy and the providers who treat them.
Another healthcare disparity relates to access to state-of-the-art comprehensive epilepsy care for patients who live in rural communities, where hospitals don’t have the resources to treat specialized care needs.7 Telehealth has the potential to transform and advance epilepsy care in a rural population of patients. Because of these insights, we recently partnered with Dr. Marvin Rossi on expanding access to telehealth services for patients with epilepsy in the state of Illinois. Signed earlier this year by Governor J.B. Pritzker, the new law will help maintain the availability of telehealth services for epilepsy patients on Medicaid through the reimbursement of healthcare providers for those services. Our proximity to patients and legitimacy within neurology has allowed us to partner better with patients as we test and iterate, helping create services to improve their care journey.
With nearly 30 years of experience in epilepsy, UCB can and will unlock what’s possible for the millions of people living with epilepsy, so their reality can be free from seizures and the other debilitating and unpredictable impacts of the disease. Our ambition is to impact the underlying causes of the disease and to discover, develop, and deliver highly differentiated medicines that will transform and, ultimately, cure the disease, so that people living with epilepsy can live their ideal life, every day.
###
US-P-DA-EPI-2100158
References:
1.Strzelczyk A, Schubert-Bast S. Expanding the Treatment Landscape for Lennox-Gastaut Syndrome: Current and Future Strategies. CNS Drugs. 2021;35(1):61-83.
2.Arzimanoglou A, French J, Blume WT, et al. Lennox-Gastaut syndrome: a consensus approach on diagnosis, assessment, management, and trial methodology. Lancet Neurol. 2009;8(1):82-93.
3.Data on file, Zogenix, Inc. 2021.
4.Centers for Disease Control. Epilepsy Data and Statistics. https://www.cdc.gov/epilepsy/data/index.html. Accessed 9 November 2021.
5.United States Census Bureau. U.S. population. https://www.census.gov/. Accessed 9 November 2021.
6.United States Census Bureau. Race and Ethnicity in the United States: 2010 Census and 2020 Census. https://www.census.gov/library/visualizations/interactive/race-and-ethnicity-in-the-united-state-2010-and-2020-census.html. Accessed 9 November 2021.
7.Gregerson, C., Bakian, A. V., Wilkes, J., et al. Disparities in Pediatric Epilepsy Remission Are Associated With Race and Ethnicity. Journal of Child Neurology. 2019;34(14): 928–936. https://doi.org/10.1177/0883073819866623
8.Nathan, C. L., & Gutierrez, C. FACETS of health disparities in epilepsy surgery and gaps that need to be addressed. Neurology Clin Practice. 2018;8(4):340–345. https://doi.org/10.1212/CPJ.0000000000000490
9.Data on File, UCB, Inc. UCB Hispanic CARES Research, 2021.
10.American Progress 2019:American Progress 2019: https://www.americanprogress.org/article/rural-hospital-closures-reduce-access-emergency-care/. Accessed November 17, 2021.
Choose Country
- Global Site – English
- Australia – English
- België – Engels
- Belgique – Anglais
- Brasil – Português
- България – Български
- Canada – English
- Canada – Français
- 中国 – 中文
- Česká Republika – Angličtina
- Danmark – Engelsk
- Deutschland – Deutsch
- France – Français
- España – Español
- Ελλάδα – Ελληνικά
- India – English
- Ireland – English
- Italia – Inglese
- 日本 – 日本語
- Казахстан – ағылшын тілі
- 한국 – 한국어
- Luxembourg – Anglais
- Luxemburg – Engels
- Magyarország – Angol
- México & Latinoamérica – Español
- Nederland – Engels
- New Zeeland – English
- Norge – Engelsk
- Österreich – Deutsch
- Polska – Polski
- Portugal – Inglês
- România – Engleză
- Россия – Русский
- Slovensko – Anglický
- Suomi – Englanti
- Sverige – Engelska
- Schweiz – Deutsch
- Suisse – Français
- Türkiye – Türkçe
- Україна – Англійська
- United Kingdom – English
- U.S.A. – English