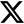Every three seconds a fragility fracture occurs. But when someone has a bone break it may not just be a part of getting older. Often, it is due to the underlying condition of osteoporosis. And when this happens, people may not always get screened for their bone health and different aspects of their care may not always be coordinated.
According to the National Osteoporosis Foundation, about 54 million Americans have osteoporosis and low bone mass, placing them at increased risk for osteoporosis. But only 9% of patients receive a Bone Mineral Density test following a new osteoporotic fracture and only 23% of patients who suffer a hip fracture receive treatment to reduce future fractures.*
The UCB Bone Health Team works with healthcare partners, including hospitals, integrated delivery systems, and community partners, to create a better system for osteoporosis care driven by what patients want and need.
Our Regional Care Leads have worked with 64 hospitals to improve their fracture prevention programs and processes and completed more than 140 assessments of the osteoporotic patient journey with hospital systems across the U.S.1 As a result, more than 150,000 patients across the U.S. have benefited from the implementation of optimized care processes.
To do this, UCB uses a model for improved care focused on working with stakeholders across healthcare organizations to improve the patient journey. Through education, assessment, planning, and collaboration we help elevate care for patients with fragility fractures.
One example of our team and model in action has been work over the past year and a half with a large health system with hospitals that initially did not have formal post-fracture care programs or processes in place. When we had the opportunity to engage the orthopedic leads at the system’s flagship hospital, we shared our knowledge about the serious care gaps that exist for patients after a fragility fracture, in addition to solutions, such as fracture liaison services (FLS) and other post-fracture care programs. During our first meeting, a physician champion stepped up and agreed it was time for the hospital and the system to act, thereby ensuring underlying bone health was proactively addressed for patients suffering from osteoporotic fractures. From there, a multidisciplinary team of relevant stakeholders was assembled that used evidence-based guidelines to help develop a post-fracture care protocol for the flagship hospital. Their goal was to prevent future fractures by addressing underlying bone health, thereby achieving the best outcomes for their osteoporosis patient population.
Ultimately, the system implemented new pathways and infrastructure to support this vulnerable patient population. These processes help ensure that any patient over age 50 admitted with a non-traumatic fracture is receiving necessary follow-up care to include a bone health evaluation, education, lab work, imaging fall risk assessment and osteoporosis treatment. Additionally, patients are connected to community-based fall prevention resources to help ensure they do not sustain another fracture. The impact of this change across the local ecosystem will improve access to quality care for over 1,100 patients with fractures caused by osteoporosis.1
“It just feels good to know that you’re contributing to change at an organizational level that will touch the lives of so many people,” said Marjorie Fox, Regional Care Lead, UCB.
The combination of focusing on patients and connecting disconnected care teams is preventing additional fractures and their consequences. At UCB, everything we do is focused on helping patients live their best lives, now and into the future.
*UCB is a supporter of the National Osteoporosis Foundation and the National Bone Health Policy Institute.
1UCB Data on File. May 2021.
Choose Country
- Global Site – English
- Australia – English
- België – Engels
- Belgique – Anglais
- Brasil – Português
- България – Български
- Canada – English
- Canada – Français
- 中国 – 中文
- Česká Republika – Angličtina
- Danmark – Engelsk
- Deutschland – Deutsch
- France – Français
- España – Español
- Ελλάδα – Ελληνικά
- India – English
- Ireland – English
- Italia – Inglese
- 日本 – 日本語
- Казахстан – ағылшын тілі
- 한국 – 한국어
- Luxembourg – Anglais
- Luxemburg – Engels
- Magyarország – Angol
- México & Latinoamérica – Español
- Nederland – Engels
- New Zeeland – English
- Norge – Engelsk
- Österreich – Deutsch
- Polska – Polski
- Portugal – Inglês
- România – Engleză
- Россия – Русский
- Slovensko – Anglický
- Suomi – Englanti
- Sverige – Engelska
- Schweiz – Deutsch
- Suisse – Français
- Türkiye – Türkçe
- Україна – Англійська
- United Kingdom – English
- U.S.A. – English